文章信息
- 魏景景, 郝莉莉, 王红霞, 康洪昌, 王威, 岳妍
- WEI Jingjing, HAO Lili, WANG Hongxia, KANG Hongchang, WANG Wei, YUE Yan
- 穴位埋线结合健脾疏肝法治疗肝郁脾虚证腹泻型肠易激综合征疗效观察及安全性评价
- Clinical observation and safety evaluation of acupoint embedding combined with soothing the liver and strengthening the spleen in the treatment of irritable bowel syndrome-diarrheal of liver depression and spleen deficiency
- 天津中医药, 2021, 38(5): 620-624
- Tianjin Journal of Traditional Chinese Medicine, 2021, 38(5): 620-624
- http://dx.doi.org/10.11656/j.issn.1672-1519.2021.05.16
-
文章历史
- 收稿日期: 2020-12-20
作为消化系统的常见病和多发病,肠易激综合征(IBS)是一种包括腹部不适或腹痛伴随排便习惯改变和(或)大便性状异常等在内的功能性肠病[1],临床可见腹泻型、便秘型、混合型及未分型,其中以腹泻型(IBS-D)最为多见[2]。其发病率较高,西方国家达10%~15%,且好发于45岁以下的中青年,而亚洲国家则稍低,为6.5%~10.1%,并呈逐年上升趋势[3]。该病症状缠绵,在大幅降低患者生活质量的同时消耗大量医疗资源[4]。当前西医以对症治疗为主,但尚无优效治疗方案[5];而中医则将其纳入“泄泻”讨论范畴,肝郁脾虚是其主要证型[6],治疗涉及内治法、外治法及内外结合等[7]。本研究采用穴位埋线结合健脾疏肝法治疗肝郁脾虚证IBS-D,报道如下。
1 临床资料 1.1 一般资料选取2018年4—6月间天津中医药大学第一附属医院消化科门诊及病房符合筛选标准的患者40例。按照随机数字表进行分组,每组各20例。两组患者在性别、年龄、病程等方面比较无统计学差异(P>0.05),具有可比性。见表 1。
参照中华中医药学会脾胃病分会《2017肠易激综合征中医诊疗专家共识意见》[8]中肝郁脾虚证辨证分型标准。主症:腹痛即泻,泻后痛减;急躁易怒。次症:两胁胀痛;纳呆;身倦乏力。舌淡胖,可有齿痕,苔薄白;脉弦细。
1.2.2 西医诊断标准参照IBS罗马Ⅲ诊断及分型诊断标准[9]。在最近的3个月内,每月至少有3 d具有反复发作的腹痛或不适,并具有下列中的2项或2项以上:排便后症状改善;排便频率的改变;粪便性状的改变。IBS-D:稀便(糊状便)或水样便比例大于等于25%;硬便或块状便比例小于25%。
1.3 纳入标准1)符合IBS-D中西医诊断。2)年龄介于18~60岁。3)受试者或家属知情同意并签署同意书。
1.4 排除标准1)其他类型IBS患者。2)伴消化道器质性病变。3)哺乳期及妊娠妇女。
2 治疗方案两组患者均予中药汤剂口服,治疗组加用穴位埋线。
2.1 中药组方炒白术30 g,白扁豆10 g,党参10 g,山药20 g,茯苓30 g,炙甘草10 g,砂仁6 g,白芍20 g,柴胡10 g,郁金10 g,陈皮10 g,薏苡仁30 g,防风10 g。早晚各150 mL。连续服用2周。
2.2 穴位埋线1)穴位:合谷(双)、天枢(双)、足三里(双)、上巨虚(双)、三阴交(双)、太冲穴(双)。2)操作:局部皮肤常规消毒后,将0号羊肠线剪至10~15 mm,装入9号埋线穿刺针内。术者一手两指绷紧或提捏穴位皮肤,另一手直刺进针约15~25 mm。针刺得气后,将针芯迅速推至针尖,使羊肠线植于皮下组织或肌肉,待完全出针贴敷创可贴。每周1次,连续治疗2周。
3 观察指标 3.1 安全性指标治疗前后分别检测血常规、肝功能,密切关注并记录受试者发生的不良反应、不良事件及严重不良事件。
3.2 疗效指标 3.2.1 IBS症状严重程度(IBS-SSS)量表分值低于75分视为缓解期,75~175分为轻度,175~300分为中度,300分以上为重度。其临床疗效等级评定如下:痊愈:积分小于75分;显效:改善2个级别;有效:改善1个级别;无效:无改善或变差[8]。
3.2.2 中医症状分级量化积分参照《中药新药研究指导原则》[10](2002版)。依据患者主症及次症严重程度分别计0、2、4、6分及0、1、2、3分,计算总计分减分率并判定疗效,具体如下:治愈:临床症状、体征消失或基本消失,积分减少≥95%;显效:临床症状、体征明显改善,积分减少≥70%;有效:临床症状、体征明显改善,积分减少≥30%;无效:临床症状、体征均无明显改善,甚或加重,积分减少不足30%。
3.2.3 IBS生活质量(IBS-QOL)量表[8]分别计算总积分和各维度积分,并按照相关公式换算标准分。标准分=(各条目实际得分和-理论最低分/理论得分范围)×100%。
3.2.4 血清5-羟色胺(5-HT)含量采用荧光分光光度法(Fluoresc-ence Spectrophotometry)分别检测两组患者治疗前后血清5-HT含量。
4 统计学方法利用SPSS 24.0进行数据分析。计量资料用均数±标准差(x±s)描述,组内前后比较采用配对t检验,组间比较采用两独立样本t检验;计数资料组间比较采用卡方检验。P<0.05表示差异有统计学意义。
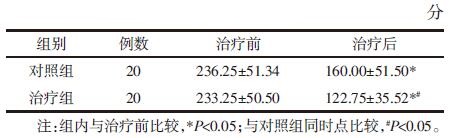
5 研究结果 5.1 IBS-SSS量表评分比较两组治疗后IBS-SSS量表评分均低于治疗前(P<0.05),且治疗组低于对照组(P<0.05)。见表 2。
|
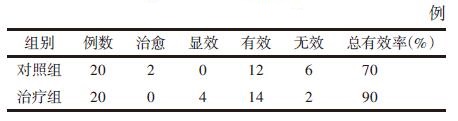
对照组痊愈2例,显效0例,有效12例,无效6例;治疗组痊愈0例,显效4例,有效14例,无效2例。治疗组优于对照组,差异无统计学意义(P > 0.05)。见表 3。
|
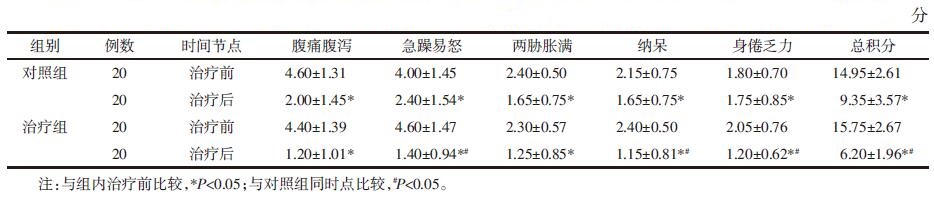
经治疗两组中医辨证症状分级计分均降低(P<0.05);同时治疗组在急躁易怒、纳呆、身倦乏力及总计分方面均低于对照组(P<0.05)。见表 4。
|
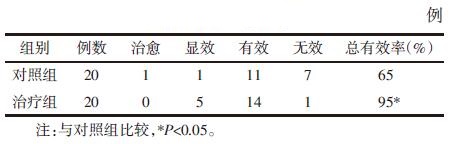
治疗组治愈0例,显效5例,有效14例,无效1例;对照组治愈1例,显效1例,有效11例,无效7例。治疗组优于对照组(P<0.05)。见表 5。
|
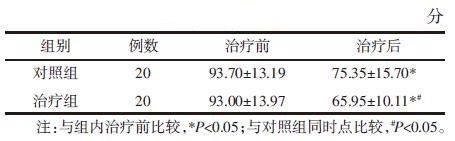
治疗后两组IBS-QOL评分均降低(P<0.05);且治疗组优于对照组(P<0.05)。见表 6。
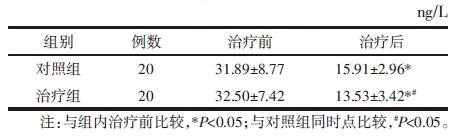
治疗后两组血清5-HT含量均降低(P<0.05);且治疗组低于对照组(P<0.05)。见表 7。
|
两组患者在治疗期间血常规、肝功能均未出现异常,且无明显不良反应及不良事件。
6 讨论IBS-D作为临床最常见的IBS分型,其致病因素较多,发病机制也尚未明确。中医多以“泄泻”“腹痛”论述,对其病因病机的认识相对统一。《医学求是》中清代医家吴达提出“木郁不达,风郁不达,风木冲击而贼脾土,则痛与脐下”的观点。明代吴鹤皋于《医方考》中言:“泻责之于脾,痛责之于肝,肝责之实,脾责之虚,脾虚肝实,故令痛泻。”认为肝郁脾虚是其发病关键[11]。而现代医家中,李军祥教授[12]将其病机归纳为脾虚肝旺,自拟痛泻安肠方治以抑肝扶脾,每获良效;叶松教授[13]亦从肝脾论治,以痛泻要方加味调和肝脾,疗效确切。或饮食不节,或情志失常,亦或感受外邪,致脏腑虚弱,继而脾失运化及大肠传导失职。又脾虚日久致肝气郁滞,肝郁反乘脾,终致肝脾失和发为本病。
针对其病因病机,本研究以参苓白术散健脾渗湿以固中州,合痛泻要方补脾柔肝,祛湿止泻,脾肝同治,标本兼顾。方中白术用量较大,味甘苦且性温燥,功专燥湿健脾,助脾胃之健运以生化。白芍味酸而性柔润,主入肝经,长于养肝血,护肝阴,敛肝气,令气不妄行。两药相伍行柔肝健脾之效。茯苓长于渗湿而益脾,白术长于健脾而燥湿。脾喜燥恶湿,两药合用,燥渗相济,除水湿而健脾气,脾气健则水湿运。防风可升举阳气,亦可胜湿。《脾胃论》云:“阳本根于阴,惟泻阴中之火,味薄风药,升发以伸阳气,则阴气不病,阳气生矣。”防风正寓此意,与炒白术共奏健脾胜湿,升举阳气之效。陈皮理气燥湿,醒脾和胃。薏苡仁有增强渗湿之功。柴胡、郁金加大疏肝力气之度。大枣性属甘温,取其补益气血,健脾和胃之效,又可调和诸药,兼有佐药兼使药之意。相关系统评价提示,参苓白术散可有效改善IBS-D患者症状及体征,缩短疗程,减轻疼痛,同时减少后遗症[14];而痛泻要方则能多靶点、多层次干预IBS-D起效[15-16]。穴位埋线疗法作为一门融合针灸经络理论和西医手段的新型学科,通过长期有效地刺激穴位达到预防和治疗疾病的效果。其临床应用广泛,尤其对某些慢性病及疑难病症,屡获奇效。本研究选穴以手阳明大肠经和足厥阴肝经为主:天枢为大肠经之募穴,位处脐旁两寸,恰似人身之中点,为清浊升降之枢纽,奏健脾和胃、通调肠腑之效。《针灸甲乙经》曰:“腹胀满病……寒邪不化,天枢主之。”配合大肠之下合穴上巨虚,调理肠腑而止泻。足三里为胃之下合穴,调脾胃而扶正祛邪。同时现代研究证实,针刺足三里可通过促进肠道蠕动,调节多种消化酶分泌,维持胃肠道功能正常[17-18]。三阴交为足三阴经之会,其功效甚多,可同调肝脾肾,兼有安神之效,能缓解腹痛、腹胀。太冲,足厥阴肝经之原穴,疏肝而解郁,合谷为大肠经原穴,善调理腑气,主治泄泻。
由结果可知,在IBS-SSS量表评分、中医辨证症状分级计分和临床疗效以及IBS-QOL评分方面,两组患者治疗后均优于治疗前(P<0.05),且组间比较显示,治疗组均优于对照组(P<0.05)。同时,治疗后治疗组患者血清5-HT含量低于对照组(P<0.05),从而验证了5-HT在激发肠道蠕动及促进分泌中发挥重要作用[19-20]。虽然IBS-SSS临床疗效比较两组没有显著差异,但是治疗组的疗效显示出优于对照组的趋势,有待于我们扩大样本量进一步研究。
综上所述,穴位埋线结合健脾疏肝法可有效降低肝郁脾虚证腹泻型肠易激综合征患者IBS-SSS及中医辨证症状分级计分,提高临床有效率及IBS-QOL评分,改善生活质量,同时降低血清5-HT含量,且无不良反应。进一步提示其可作为该病临床治疗的可靠选择,但因本研究存在样本量较少,疗程较短等不足,故仍需大样本、多中心研究进一步验证其近远期疗效及安全性。
| [1] |
中华医学会消化病学分会. 肠易激综合征诊治的共识意见[J]. 中华内科杂志, 2003, 42(9): 669-670. Chinese Society of Gastroentnrology. Consensus views on diagnosis and treatment of irritable bowel syndrome[J]. Chinese Journal of Internal Medicine, 2003, 42(9): 669-670. DOI:10.3760/j.issn:0578-1426.2003.09.036 |
| [2] |
胡品津, 潘国宗. 中华医学会第一届全国肠易激综合征学术会议纪要[J]. 中华消化杂志, 2003, 23(7): 428. HU P J, PAN G Z. Summary of the first national conference on irritable bowel syndrome held by the Chinese Medical Association[J]. Chinese Journal of Digestion, 2003, 23(7): 428. |
| [3] |
CHANG F Y, LU C L, CHEN T S. The current prevalence of irritable bowel syndrome in Asia[J]. Journal of Neurogastroenterology and Motility, 2010, 16(4): 389-400. DOI:10.5056/jnm.2010.16.4.389 |
| [4] |
SCHNRICH S, BROCKOW T, FRANKE T, et al. Analyzing the content of outcome measures in clinical trials on irritable bowel syndrome using international classification of functioning disability and health as a reference[J]. Rehabilitation (Stuttg), 2006, 45(3): 172-180. DOI:10.1055/s-2005-915277 |
| [5] |
卢璐, 袁建业, 费晓燕, 等. 肠易激综合征发病机制研究及治疗进展[J]. 中国中西医结合消化杂志, 2015, 23(9): 661-664. LU L, YUAN J Y, FEI X Y, et al. Progress in the pathogenesis and treatment of irritable bowel syndrome[J]. Chinese Journal of Integrated Traditional and Western Medicine on Digestion, 2015, 23(9): 661-664. |
| [6] |
汪红兵, 张声生, 李振华, 等. 360例腹泻型肠易激综合征的主要证候分布与不同因素关系的研究[J]. 中国中医药信息杂志, 2010, 17(3): 18-20. WANG H B, ZHANG S S, LI Z H, et al. Study on relationship between the main symptoms' distribution and different factors of 360 cases of IBS-D[J]. Chinese Journal of Information on Traditional Chinese Medicine, 2010, 17(3): 18-20. DOI:10.3969/j.issn.1005-5304.2010.03.008 |
| [7] |
王文, 张莎, 朱芳红. 肠易激综合征的中医药治疗现状及分析[J]. 中国中医急症, 2020, 29(4): 750-752. WANG W, ZHANG S, ZHU F H. Status and analysis of traditional Chinese medicine treatment of irritable bowel syndrome[J]. Journal of Emergency in Traditional Chinese Medicine, 2020, 29(4): 750-752. DOI:10.3969/j.issn.1004-745X.2020.04.054 |
| [8] |
张声生, 魏玮, 杨俭勤, 等. 肠易激综合征中医诊疗专家共识意见[J]. 中医杂志, 2017, 58(18): 1615-1620. ZHANG S S, WEI W, YANG J Q, et al. Consensus on standard management of irritable bowel syndrome in TCM[J]. China Journal of Traditional Chinese Medicine and Pharmacy, 2017, 58(18): 1615-1620. |
| [9] |
姚欣, 杨云生, 赵卡冰, 等. 罗马Ⅲ标准研究肠易激综合征临床特点及亚型[J]. 世界华人消化杂志, 2008, 16(5): 563-566. YAO X, YANG Y S, ZHAO K B, et al. Clinical features and subtype of irritable bowel syndrome based on Roman Ⅲ diagnostic criteria[J]. World Chinese Journal of Digestology, 2008, 16(5): 563-566. DOI:10.3969/j.issn.1009-3079.2008.05.023 |
| [10] |
郑筱萸. 中药新药临床研究指导原则(试行)[M]. 北京: 中国医药科技出版社, 2000. ZHENG X Y. Guiding principles for clinical research of new Chinese medicines (trial)[M]. Beijing: China Medical Science Press, 2000. |
| [11] |
陈婷, 唐旭东, 王凤云, 等. 腹泻型肠易激综合征中医辨证的源流及发展趋势[J]. 中华中医药杂志, 2015, 30(8): 2671-2674. CHEN T, TANG X D, WANG F Y, et al. Origin and development of IBS-D based on TCM syndrome differentiation[J]. China Journal of Traditional Chinese Medicine and Pharmacy, 2015, 30(8): 2671-2674. |
| [12] |
谭祥, 裴文婧, 谢春娥, 等. 李军祥教授辨治腹泻型肠易激综合征经验[J]. 中国中西医结合消化杂志, 2019, 27(10): 788-789. TAN X, PEI W J, XIE C E, et al. Professor LI Junxiang's experience in distinguishing and treating diarrhea-type irritable bowel syndrome[J]. Chinese Journal of Integrated Traditional and Western Medicine on Digestion, 2019, 27(10): 788-789. |
| [13] |
刘静, 叶松, 胡运莲, 等. 叶松教授从肝脾论治腹泻型肠易激综合征经验[J]. 亚太传统医药, 2020, 16(6): 112-114. LIU J, YE S, HU Y L, et al. Professor YE Song's experience in treating irritable bowel syndrome with predominant diarrhea from liver and spleen[J]. Asia-Pacific Traditional Medicine, 2020, 16(6): 112-114. |
| [14] |
于莹, 张功, 黄海量, 等. 参苓白术散治疗腹泻型肠易激综合征系统评价[J]. 山东中医药大学学报, 2017, 41(1): 18-23. YU Y, ZHANG G, HUANG H L, et al. Systematic evaluation of Shenling Baizhu Powder in the treatment of diarrheal irritable bowel syndrome[J]. Journal of Shandong University of Traditional Chinese Medicine, 2017, 41(1): 18-23. |
| [15] |
马祥雪, 王凤云, 张北华, 等. 痛泻要方治疗腹泻型肠易激综合征的作用机制研究现状与思考[J]. 世界中医药, 2015, 10(7): 977-981. MA X X, WANG F Y, ZHANG B H, et al. Research status and thoughts of Tongxie Yaofang's pharmacological mechanisms for diarrhea-predominant irritable bowel syndrome[J]. World Chinese Medicine, 2015, 10(7): 977-981. DOI:10.3969/j.issn.1673-7202.2015.07.003 |
| [16] |
姚鹏. 四逆散合痛泻要方与西药治疗肠易激综合征疗效系统评价[J]. 天津中医药, 2016, 33(5): 279-284. YAO P. Evaluation on the therapeutic effect of Sini powder and Tongxieyao prescription and Western medicine on irritable bowel syndrome[J]. Tianjin Journal of Traditional Chinese Medicine, 2016, 33(5): 279-284. |
| [17] |
朱丽丽, 杨丽明, 刘秋萍, 等. 足三里穴位埋线促进腹部术后胃肠功能恢复的效果研究[J]. 中国医药导报, 2010, 7(18): 25-26. ZHU L L, YANG L M, LIU Q P, et al. Effect of catgut implantation at Zusanli acupoint on promoting gastrointestinal functional rehabilitation after abdominal operation[J]. China Medical Herald, 2010, 7(18): 25-26. DOI:10.3969/j.issn.1673-7210.2010.18.011 |
| [18] |
魏景景, 周正华. 腹泻型肠易激综合征中医外治法研究进展[J]. 天津中医药, 2018, 35(2): 157-160. WEI J J, ZHOU Z H. Research progress of Chinese medicine external treatment of diarrhea predominant irritable bowel syndrome[J]. Tianjin Journal of Traditional Chinese Medicine, 2018, 35(2): 157-160. |
| [19] |
陈奕霞, 王海燕, 邓素萍. 四逆散合痛泻要方加味对肠易激综合征患者血清5-羟色胺表达水平的影响研究[J]. 检验医学与临床, 2014, 11(11): 1462-1464. CHEN Y X, WANG H Y, DENG S P. Clinical research on effects of Sinisanhetong decoction on 5-HT in patients with irritable bowel syndrome[J]. Laboratory Medicine and Clinic, 2014, 11(11): 1462-1464. DOI:10.3969/j.issn.1672-9455.2014.11.005 |
| [20] |
COOKE H J. Neurotransmitters in neuronal reflexes regulating intestinal secretion[J]. Annals of the New York Academy of Sciences, 2000, 915: 77-80. |
 2021, Vol. 38
2021, Vol. 38